Right now is not so good. I’m going to be pretty frank, but I don’t want people to worry. I’ve been through some bad brain stuff even before Roscoe took over my life, and even when I’m close to the bottom of the deep well of suckitude, I can still remember to look up to the light at the top and know there’s a way up as well as a way down.
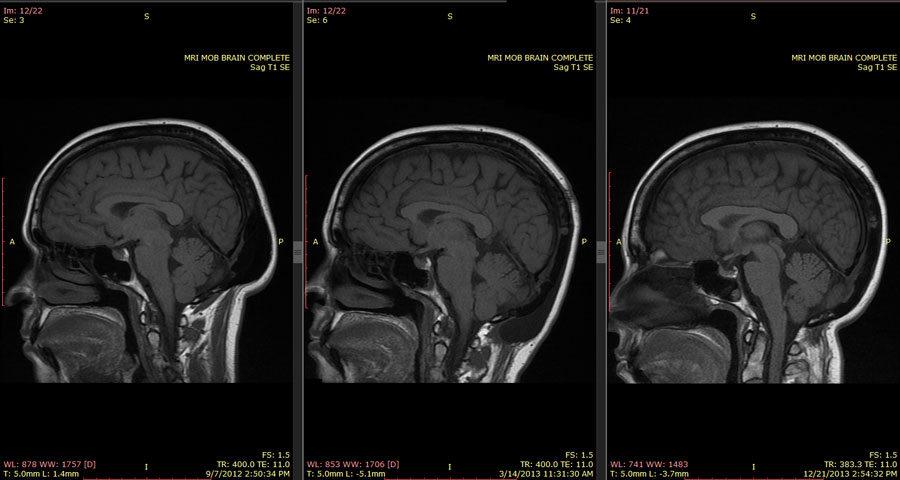
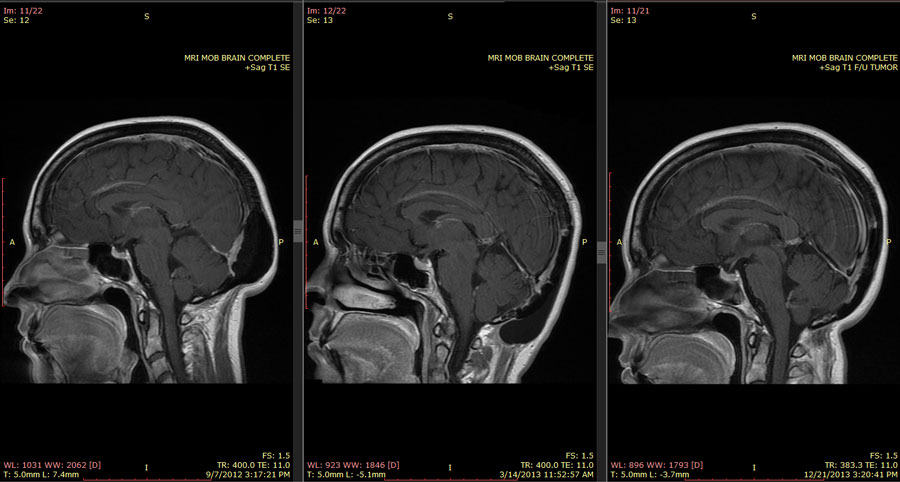
My medications aren’t working the same way as they did before, which is no surprise. If you look at the early MRIs, there was a lot of compression. Blood supply was rerouted or restricted. Neurons were obviously going to be moving around trying to get past blockages. And the limbic system, where most of our emotions are seated, was pretty wonky from getting pushed out of shape. So this is just like starting all over again from scratch. Cymbalta is too stimulating an antidepressant because it’s a norepinephrine reuptake inhibitor, meaning that my whole “fight or flight” reaction is on higher alert than it should be. I also had to discontinue Adderall for the same reason, and add in Klonopin because my life had become all panic, all the time.
When you’re transitioning from one antidepressant to another, there’s this horrible period during which you’re getting too little of both of them. That’s where I’m at right now. I’m titrating down on Cymbalta – 15mg per day. This is enough to reduce the panic and keep the brain zaps to a minimum, but not enough to affect my depression. At the same time, I’m beginning sertraline (Zoloft) but only a measly dose of 25mg. Not only not enough to even tickle the edges of depression, but also only starting the 4-6 week journey before it shows any effect whatsoever. In a few days I’ll be off the Cymbalta (protip – it’s a capsule full of beads, so if you feel a brain zap, and ONLY if you feel a brain zap, take one or two BEADS. Makes it less awful.) and up to 50mg of sertraline. Still a baby dose, and still at least two weeks away from making even a tiny bit of difference.
So, yeah, I’m in a pretty bad way right now. Fortunately, even when a smidgen of suicidal ideation pops up, it’s easily quashed by reminding myself of the light at the top of the well of suckitude and by making a plan so elaborate (typical ADHD) that I’d decide it was too much effort before I even came close to doing anything about it. No matter what I might say in the throes of depressive misery, you’re not going to get rid of me that easily. Heh.
The whipped cream and cherry on top is the visit to the neurosurgeon. My brain, right now, is about as good as it’s going to get. I’m going to see a neuropsychologist for an evaluation, and probably end up with some kind of therapy to help me adapt to my new neurological paradigm, but I was kind of hoping for normal. Having that hope dashed is not helping with my mood. Yes, I’m way, way better than I was two years ago, but there are things that are a struggle still.
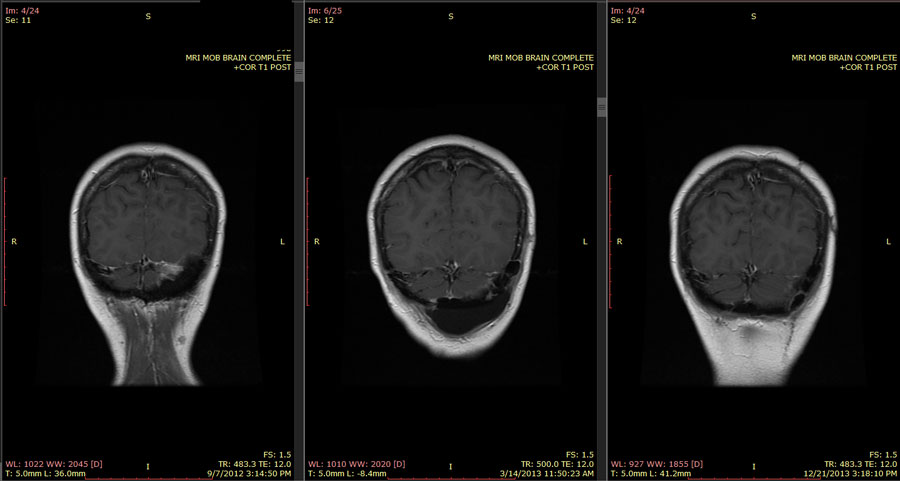
My spatial relations are vastly improved – I have a much better concept of where I am in the space that surrounds me, I have my sense of direction back, and I’m aware of objects around me, both moving and stationary. However, “mirror images,” both literally (myself in the mirror) and figuratively (looking at pictures or looking at other people) are bizarre and confusing. I have trouble telling right from left, and forwards from backwards. Up and down are intact, thank goodness. Blow drying my hair has been an adventure, and I still haven’t quite mastered the art of flossing my teeth without hurting myself. If I look at my MRIs, I have to pretend that they are someone else’s, because their orientation is like a mirror, and they start from the far side and come forward. If I think of them as mine, I can’t get past the idea that my left side is on the right of the image, and the coronal slices as they move from the back of my head to the front are coming towards me instead of moving away from me.
I don’t lose my balance all that much anymore, either. . .but it still happens.
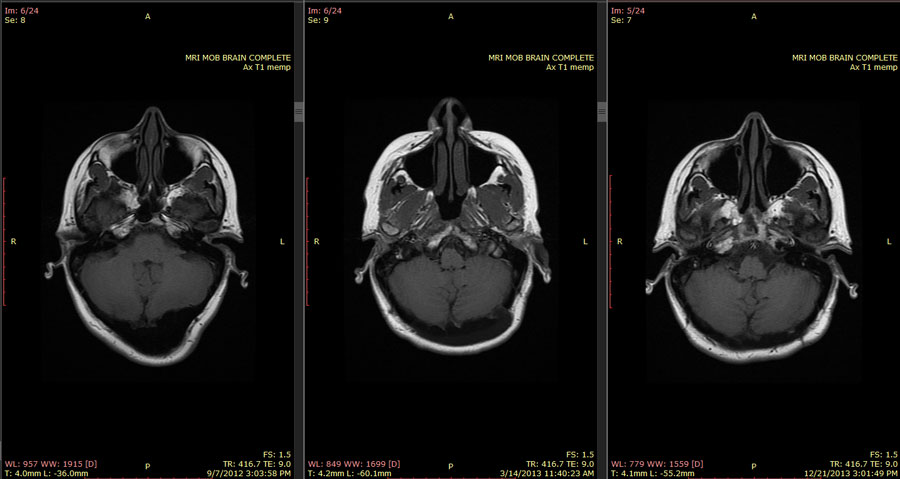
Since the tumor smooshed my left occipital lobe and left temporal lobe, I also have some problems that are related to vision and vision-related language performance. I don’t have any consistent object or color blindness, but sometimes I will look at things, see them, but not really “recognize” them, or know what they are. Quick example – we were at a food kiosk, and I wanted to leave a tip. There was a bright blue tip cup by each cash register. On the one that was right in front of my face, I couldn’t see the word “tips” written on it. I saw only the “s” and thought for some reason that it meant that was a cup for straws. So I reached over and put the tip in the cup on the other side of the kiosk, because I could perceive the whole word on that one. Other times, I won’t see things outside of what I’m looking at because I simply don’t understand why the thing I’m looking at isn’t the thing I want. Really. I look at it, and I think “this isn’t what I want? Why isn’t it what I’m looking for?” and the thing I want is right there above it or below it or next to it.
The most frustrating thing, though, is the anomia. This is where the temporal lobe gets involved. Most of your language processing occurs in your left temporal lobe, and the normal loop between seeing something and saying it involves the visual image that’s processed somewhere in your right hemisphere (depending on what it is) being “translated” by your left occipital lobe and sent into the language loop in your temporal lobe. That’s not happening for me. But only in one direction. If I see an object or a person (or picture an object or person in my head) there’s a good chance that I will not be able to name that object or person. I could tell you everything about that object or person that I knew, except for what that object or person is called. And the name I remember this morning may well be completely inaccessible in a few hours. No amount of prompting, besides actually telling me the word, is going to bring that name into my conscious thoughts.
In the other direction, no problem. If I hear or read a noun or a name, I have no trouble whatsoever picturing that object or person in my mind. But it is kind of a problem – because when I’m circumlocuting to try to use the words I have to describe the word I don’t, people try to be helpful and finish my sentences for me. And once they say the word that isn’t the one I’m looking for, it creates a new mental image that supersedes the one I’m trying to describe, and all is lost. I know they’re trying to be helpful, and I know it’s awfully difficult to listen to me when I’m struggling through this, but really, the only thing it accomplishes effectively is to make me feel like crap and maybe even start crying. Just a heads up. I won’t hold it against you, I promise, but I will probably start to cry.
So. . .I see the psychiatrist in another couple of weeks and we’ll ramp up the sertraline if it’s working OK. I may even be able to go back on Adderall once my dose is stabilized. We’re looking at mid-March here. If you’re worried about my mood, look at your calendar. If it isn’t halfway through March, stop worrying. I’m just transitioning between medications.
February 11th, I go for a consult with the neuropsychologist, and get another dose of reality about how much improvement, if any, I can expect with therapy. Until then, I have regressed to the mean, and everything I just described above is SOP. And that’s just the way it is.